
Fall of the assisted dying Bill: We cannot lose focus on palliative and end of life care

Toby Porter, CEO of Hospice UK, responds to the fall of the assisted dying Bill in England and Wales by highlighting the need for continued focus on palliative and end of life care, so everyone can get the care they need.
Today, we know for certain that Assisted Dying will not become legal in England and Wales at this attempt. The Terminally Ill Adults (End of Life) Bill introduced by Kim Leadbeater MP and sponsored by Lord Falconer has not passed the Committee stage in the House of Lords and therefore fails at the end of today's session.
Views on Assisted Dying are varied, often polarised and passionately held. Views about intent and process of the Bill failing due to the time taken at Lords Committee Stage will similarly almost totally split along original views on whether the law should change. One person's legislative scrutiny is another person's fillibustering, let others have the constitutional arguments and speculate whether, how and when the Bill might be re-introduced.
My role with Hospice UK has allowed me the genuine privilege of many long conversations about this subject and draft Bill with the MPs and Peers leading efforts on either side. Despite the harsh words inevitably being thrown about today as the Bill fails, I defy any neutral person not to recognise that the strongest advocates and opponents of a change in the law share an obvious and equal abundance of conviction and deep empathy for terminally ill people, and want to see better and more equitable access to palliative care nationally, including a strong and fairly funded hospice sector.
We should recognise and be grateful for the compassion and wisdom that we have seen and heard for almost eighteen months now. We should particularly celebrate the fact that the introduction and passage of this Bill, along with the similar one introduced by Liam Macarthur MSP in Scotland, has led to a sustained national conversation about death, dying, choice and dignity at the end of life.
These are profound and highly important subjects, and ones that every person alive will eventually experience for themselves. The introduction and passage of Kim Leadbeater’s Bill threw into the mainstream a question we often avoid, as individuals and as a society. What kind of death, and choice over that death, do we want people to have?
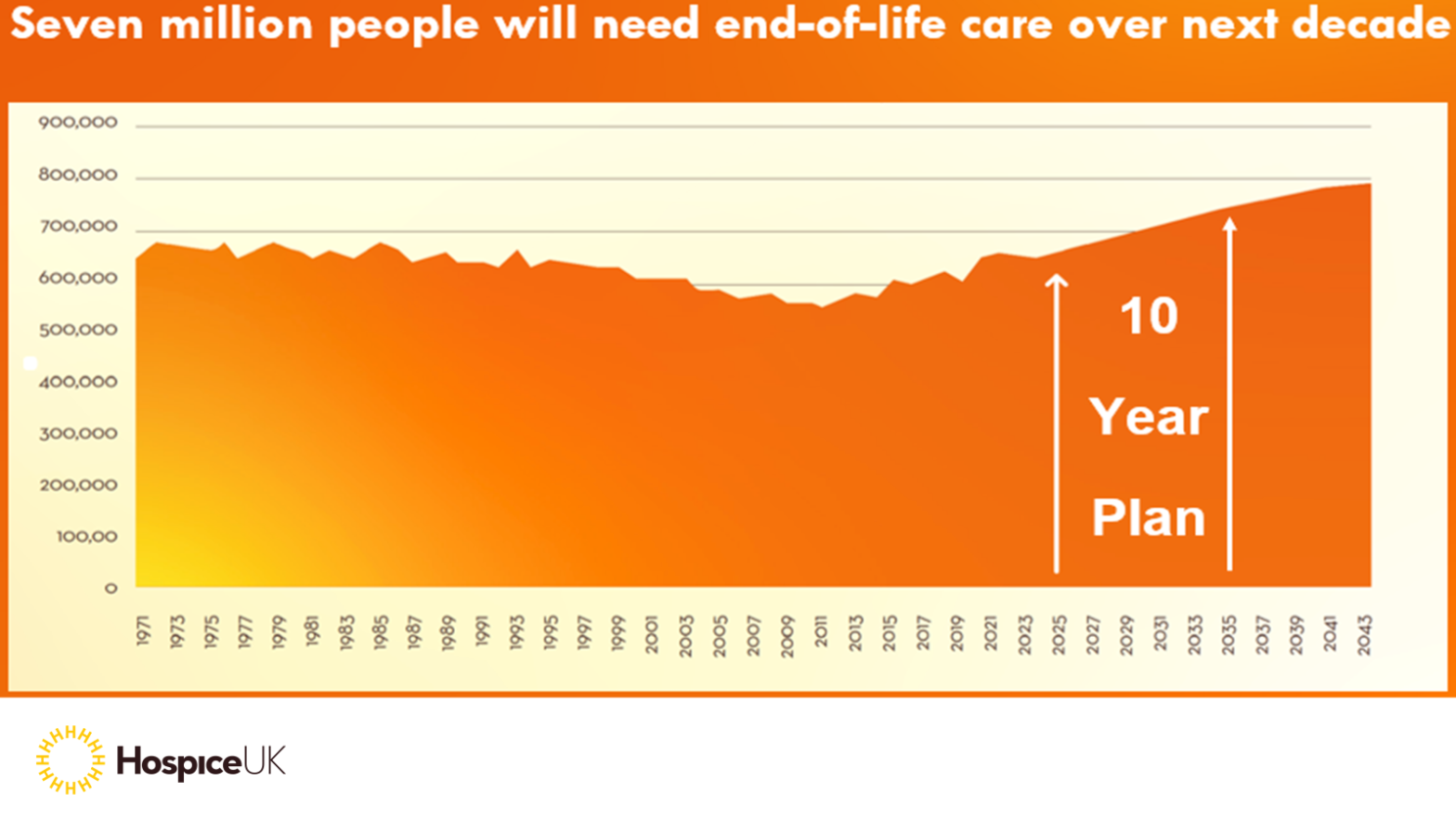
This is no academic question. All of us will die, and our rapidly ageing population means far more of us will die over coming years than ever before. For example, over the NHS’s new 10 year plan period, 7 million people in the UK are forecast to die, around a million more than over the previous decade.
The Government’s Impact Assessment published for this Bill modelled how well under 2% of the population would be expected to have an assisted death, if and when the bill pass passed and assisted dying became available in practice.
What can the 98% of us expect? The truth is that “ordinary dying” in the UK is a very mixed picture. Already, according to Marie Curie, nearly 1 in 3 people who need palliative care don’t get the support they need at the end of their lives, causing avoidable pain, distress, and heartache.
Challenges accessing palliative care are especially visible within excluded communities and groups. This of course explains the concern that opponents of the Bill have consistently highlighted of what a change in the law on Assisted Dying could mean for society’s most vulnerable members, many of whom are already marginalised from and distrustful of health and social care services and providers.
Too many people already can’t get the palliative and end of life care they need right now. We have all been shocked in recent winters to see footage of people dying in corridors in overwhelmed hospitals or hear from relatives of people who died in pain or without the dignity and privacy at the moment of death that every single one of us would view as our birthright in the world’s fifth largest economy.
There are still enormous amounts our politicians, our institutions and we all as a society can do to give as many people as possible the best death possible when the time comes. Good palliative and end of life care, available to everyone who needs it, is essential to making this a reality.
Hospice UK highlighted the risks at every opportunity for 18 months of the Bill’s passage of the moral and practical catastrophe that someone might choose an Assisted Death in the future not because they were tired of living, but because they were not able to get the high quality palliative care that they needed.
I know for a fact that the Bill sponsors wished deeply to see an investment in palliative care that would accompany the passage of the Bill. This Government has also made a serious and sustained commitment to making long-term improvements to palliative care, this feels very different and very important for our sector. The key long-term vehicle is the Modern Service Framework for Palliative and End-of-Life Care currently being developed by palliative care leads in NHS England and Department of Health and Social Care , and formally announced by Care Minister Stephen Kinnock at last year's Hospice UK conference in November.
But the heart-breaking reality is that the actual availability of this care has almost certainly shrunk further in the year and a half that first MPs and then Peers have been debating Assisted Dying, because of cost and workforce pressures in the NHS, social care and the hospice sector.
Lack of funds means nearly 6 in 10 hospices are making or considering service cuts, just when they should be expanding them. 380 desperately needed beds are out of use in English hospices as they can’t afford to staff them. Far more hospice beds closed than were opened during the passage of this Bill.
Across the UK, hospices made 150,000 fewer specialist community visits last year than previous years. Many hospices are running waiting lists and turning people away for the first time in their 30- or 40-year history.
Financial pressures on hospices means more pressure on an already fragile NHS, it means people dying in corridors, people dying without pain relief, it means more traumatised loved ones left to pick up the pieces.
The debates in Holyrood, the Senedd, the House of Commons and the House of Lords have together represented the most extraordinary, steadfast and welcome statement of support for high-quality palliative and end of life care for all, and the vital role of hospices play as part of our wider health and care system.
Whilst the two Bills will not progress, this support must continue. We must not lose focus on what makes a good death and what needs to be done to make sure everyone gets one. Opponents and supporters of the assisted dying Bill alike must now channel their energy and passion into ensuring high-quality palliative and end of life care is available to everyone who needs it, and calling for hospices to be properly funded, to be there for everyone who needs them.
The measure of the skill and values of the Government, politicians, as well as our institutions like the NHS, will be the extent to which the momentum and passion from the assisted dying Bill debate is used to transform access to palliative care for the whole UK population, especially those vulnerable and excluded groups.
We surely want to be a country where everyone gets the care they need at the end of their life, including the death they choose. Good palliative and end of life care offers people enormous choice at the end of their lives, as well as dignity, comfort, and essential support for their loved ones. We cannot let it be cut back further and further.
Over the next 15 years more people will die in the UK than ever before. Securing the future of end of life care could not be more important. But the way hospices are funded is not fit for purpose. The combination of rising costs and stagnating funding is leaving many with no choice but to cut essential services and make valued staff redundant. Ultimately it is patients who pay the price.
We’re calling on the Government to urgently implement our four-point plan for fair hospice funding, so hospices can finally begin to plan and provide their essential care free from financial worry.
This starts with committing £112.5 million in recurring revenue funding this year as the first step in fully funding the specialist palliative care delivered by hospices, so they can provide their essential care to everyone who needs it.
The hospice sector has been working flat out behind the scenes modelling the very significant impact that a change in the law would likely have had on hospices, their staff and volunteers, and their relationship with their local communities. I do not in any way consider this wasted work, we have learned something new at Hospice UK with every workshop and discussion.
Hospice UK and the wider hospice sector has been largely neutral on the principle of whether the law should change and, I hope, judicious in recognising that the fiduciary duty of advancing the best long-term interests of the charity was unlikely to be best served by directly taking sides in the public and private debates that divide our staff, volunteers and supporters, as well as the local communities we serve.
Conversely, we have always felt that pointing out the currently patchy and precarious state of palliative care and the fragility of much of the hospice sector, was where we could and should be focussing.
This Bill has failed, we don't know if, when and how it will next come back. So doesn't it make sense now for both sides to redouble their efforts to advance the most obvious and important point of unity to have emerged over the entire passage of the Bill?
That is the need for us to be a country investing seriously in wider and more equitable access to high quality, sustainably funded, palliative and hospice care. That is an achievable and highly important outcome, and in no way a controversial one.
Without in any way weakening the arguments either for or against a change in the law on Assisted Dying, transforming "ordinary" palliative care access and delivery is the action that would have the most impact on by far the greatest numbers of terminally ill people and their loved ones.
And the best thing about it is that nobody has yet said it shouldn't or couldn't be done.
- Toby Porter, CEO of Hospice UK, 24th April 2026
*Some part of this reproduced from an article in the Financial Times: We must renew palliative care focus as part of assisted dying decision – Toby Porter, Financial Times, June 2025.
